Read and report vaccine reactions, harassment and failures.
Ebola (Ebola Hemorrhagic Fever)
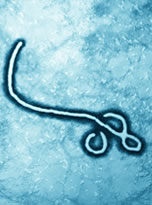
Ebola: The Disease
Ebola is a serious contagious viral disease with a high mortality rate. The natural reservoir for the virus is thought to be a fruit bat native to Africa. Both humans and non-human primates are susceptible to infection.
Symptoms start with a fever, headache, muscle and stomach pain, diarrhea, vomiting, fatigue, weakness, skin bruising and bleeding. As the disease progresses, damage to the immune system as well as the body’s internal organs occur. White blood cell and platelet counts decrease and both internal and external bleeding can occur. Fatality rates from the disease have ranged from 25 to 90 percent but the average case fatality rate is estimated at 50 percent. A person can have the virus but not show any symptoms for as long as three weeks.
Persons who survive Ebola virus disease develop long-term immunity; however, health problems frequently persist upon recovery. Learn more about ebola…
Ebola Vaccine
On December 19, 2019, the FDA approved ERVEBO (rVSV-ZEBOV), a genetically modified live Ebola virus vaccine for use in persons 18 years of age and older. This vaccine is manufactured by Merck and targets the Zaire ebolavirus strain. ERVEBO is a live, genetically modified Ebola virus vaccine and uses an attenuated vesicular stomatitis virus, a pathogen that infects livestock (cattle, horses, deer, pigs) with one of its genes replaced by an Ebolavirus gene.
Adverse events reported during clinical trials of ERVEBO included: injection site pain, swelling, and redness; headache; fever; nausea; fatigue; muscle pain; joint pain, swelling, stiffness, warmth, and redness; abnormal sweating; rash; mouth ulcers; vesicular lesions; arthralgia; arthritis; anaphylaxis; cerebrovascular accident; hemorrhagic stroke; subarachnoid hemorrhage; pulmonary embolism; and death. Learn more about ebola vaccine…
Quick Facts
Ebola (Ebola Hemorrhagic Fever)
-
Ebola is a serious contagious disease with a high mortality rate. The incubation period from initial exposure to onset of acute disease symptoms is between 2 and 21 days with the average being 8 to 10 days. Symptoms start with a fever, headache, muscle and stomach pain, diarrhea, vomiting, and skin bruising and may also include a skin rash, red eyes, and hiccups. Additional symptoms may include shortness of breath, chest pain, confusion, seizures, and bleeding. White blood cell and platelet counts decrease and both internal and external bleeding can occur. Fatal cases usually present with more severe symptoms early in the course of the illness, and death generally occurs from sepsis or multiorgan failure between day 6 and 16.
-
The Ebola virus is transmitted through direct contact with infected blood or body fluids, or by coming into contact with objects infected by the virus. It can also be spread through exposure to infected primates (apes, monkey, etc.) or fruit bats. A person with Ebola virus is only contagious to others after they begin to show signs of illness. Continue reading quick facts…
Ebola Vaccines
-
On December 19, 2019, the FDA approved Merck’s ERVEBO Ebola vaccine, a genetically modified live Ebola virus vaccine for use in persons 18 years of age and older. The vaccine targets the species Zaire ebolavirus. The CDC’s Advisory Committee on Immunization Practices (ACIP) recommends that ERVEBO be given to all persons responding to an outbreak of Ebola virus disease, healthcare workers treating patients at federally-designated Ebola treatment centers in the U.S., biosafety-level 4 laboratory personnel, healthcare personnel at specialized pathogen care centers, and to support and laboratory staff at Laboratory Response Network facilities.
-
The ERVEBO package insert reports that the vaccine has the potential to infect others with vaccine-strain Ebolavirus due to virus shedding. Continue reading quick facts…
NVIC encourages you to become fully informed about Ebola and the Ebola vaccine by reading all sections in the Table of Contents below, which contain many links and resources such as the manufacturer product information inserts, and to speak with one or more trusted health care professionals before making a vaccination decision for yourself or your child. This information is for educational purposes only and is not intended as medical advice.



