Read and report vaccine reactions, harassment and failures.
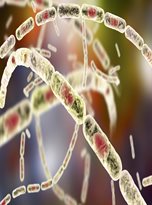
Anthrax is a serious bacterial infection caused by Bacillus anthracis. It is not contagious or spread from person to person. The bacteria produces spores that can survive for years in dry soil but can be destroyed by boiling or treating with hydrogen peroxide or dilute formaldehyde. Other methods that may be useful include bleach, chlorine dioxide gas, and a combined Ultraviolet-C light/X-ray system.
The disease most commonly occurs in animals such as cattle, sheep, horses, and goats after they graze in areas contaminated with spores of B. anthracis. The body wastes and carcasses of infected animals, or flies that eat infected carcasses, and contaminated hides and meat are all sources of anthrax.
There are three known strains of anthrax – Ames, Vollum, and Sterne. The Ames strain, considered the most virulent, was initially isolated in Texas in 1981 and found in both the U.S. and the United Kingdom.
There are four types of anthrax – Cutaneous (Skin), gastrointestinal, inhalation, and injection.
Cutaneous Anthrax
This is the most common and least deadly form of anthrax and occurs when spores enter the body through openings in the skin, such as scrapes or cuts. Infection generally occurs within one to seven days after exposure. Symptoms include bumps or blisters that may be itchy and swelling around the site. An ulcer with a black center may also form after the initial presentation. Most people who develop cutaneous anthrax become exposed by handling contaminated animal products. Most cases of cutaneous anthrax resolve without treatment and only between five and 20 percent of untreated cutaneous anthrax cases are fatal.
Inhalation Anthrax
This occurs when anthrax spores are inhaled and enter the respiratory system, with the most frequent exposure occurring during the processing of animal by-products such as hides or wool. Symptoms of inhalation anthrax are generally non-specific and can include shortness of breath, cough, fever, chills, extreme fatigue, head, and body aches, confusion, dizziness, nausea, vomiting, and stomach pain. The incubation period of the illness is about one week but can be up to 60 days.
Gastrointestinal Anthrax
While rare, gastrointestinal anthrax can occur when a person consumes raw or undercooked meat from an infected animal. It can also occur if a person swallows aerosolized anthrax spores from animal by-products. There are two forms of gastrointestinal anthrax – intestinal and oropharyngeal. Intestinal anthrax occurs when the spores cause ulcers along the intestinal tract. Symptoms of intestinal anthrax include nausea, vomiting, diarrhea, and abdominal pain. Complications include bleeding, perforation, obstruction, and shock. Oropharyngeal anthrax occurs when spores attach to the back of the throat (pharyngeal area). Symptoms of oropharyngeal anthrax can include congestion, neck swelling, and fever. The incubation period of gastrointestinal anthrax ranges from one to seven days.
Injection Anthrax
A newer form of anthrax, injection anthrax, was first identified in Northern Europe and associated with persons who inject heroin. Symptoms of injection anthrax are like cutaneous anthrax; however, the infection may occur deeper in the skin or into the muscle. No cases of injection anthrax have been identified in the U.S. Approximately 33 percent of injection anthrax cases are fatal.
Confirmation of an anthrax diagnosis can include blood antibody testing or specific testing of specimens, including respiratory secretions, spinal fluid, and skin lesions. Testing must be completed before antibiotic treatment begins. More sensitive lab tests can also be performed for anthrax disease confirmation.
Persons exposed to anthrax but have no symptoms are generally treated prophylactically for 60 days with antibiotics that include doxycycline and ciprofloxacin. Antibiotics and anthrax antitoxins are available to treat persons with symptoms of anthrax. Outcomes are better if persons receive prompt treatment as soon as symptoms develop.
IMPORTANT NOTE: NVIC “Quick Facts” is not a substitute for becoming fully informed about anthrax and the anthrax vaccine. NVIC recommends consumers read comprehensive information NVIC provides on anthrax, the vaccine manufacturer product information inserts, and speak with one or more trusted health care professionals before making a vaccination decision for yourself or your child.



