Read and report vaccine reactions, harassment and failures.
What is the History of Hib in America and Other Countries?
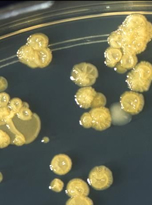
Haemophilus influenzae was first identified by Robert Pfeiffer in 1892 during an epidemic of influenza. At this time, it was believed that this bacteria was responsible for influenza. However, in 1933, influenza was determined to be caused by a virus, and H. influenzae found to be a secondary infection.
In the 1930’s, Margaret Pittman identified the two distinct types of H. influenzae, the encapsulated and unencapsulated strains. Pittman found six unique types of encapsulated strains of H. influenzae, labeling them as strains a to f, while noting type b to be the most prevalent strain found in both the blood and cerebrospinal fluid (CSF) samples that were collected. The unencapsulated strains of H. influenzae were attributed to mucosal surface infections such as conjunctivitis, otitis media, sinusitis, and bronchitis.
In December of 1982, three years prior to the introduction of the first Hib vaccines, the CDC reported invasive H. influenzae to be the leading cause of meningitis in the United States, and responsible for an estimated 8,000 to 11,000 infections per year, and fatal in three to seven percent of all cases. Infection rates were highest in children under the age of one and decreased consistently thereafter. It was also estimated that an additional 6,000 H. influenzae cases resulted in other forms of invasive disease that included bacteremia, cellulitis, epiglottis, and pneumonia. H. influenzae, however, was not a reportable disease in the United States until 1991, and infection rates were estimates tabulated from different sources throughout the country.
In 1991, the first year invasive H. influenzae became a nationally notifiable disease in the United States, there were 2,764 reported cases, with over half of the cases impacting children under the age of five. A 1998 CDC published report examining H. influenzae disease in infants and children found that in 1996-1997, of the 144 children diagnosed with Hib invasive disease, 27 had completed the recommended three-dose primary series (nearly 19 percent), and 14 (almost 10 percent) had also received a booster dose.
Between 1998 and 2000, there were 3,901 reported cases of H. influenzae, with 824 cases reported in children under the age of five. Of the 824 cases affecting children under the age of five, only 197 (24 percent) were confirmed to be the result of H. influenzae type b. One hundred and eleven of the 197 H. influenzae type b cases affected children over the age of 6 months of age and eligible to have completed the primary three doses of Hib vaccine. Of the 111 children, 35 percent had completed the primary Hib vaccine series, and over half of these children had also received a booster dose.
In 2010, there were 3,151 reported cases of H. influenzae disease, with 446 cases reported in children under the age of five. In children under the age of five, only 23 cases were confirmed as H. influenzae type b. The remaining cases were determined to be a combination of unknown and non-b serotype H. influenzae.
The burden of invasive H. influenzae disease has shifted from children to adults, and most notably to seniors 65 years of age and older. In 2011, two published studies reported on the change in the demographics of H. influenzae, with one study in particular noting that 51 percent of H. influenzae infections and 67 percent of H. influenzae related deaths occurred in adults over the age of 65. H. influenzae type b (Hib) was found to be responsible for only 9 percent of the serotyped cases, while 43 percent of cases were attributed to nontypeable H. influenzae strains. Non-b type H. influenzae, particularly types a and f, were found to be responsible for 49 percent of cases.
In 2020, there were 2,996 reported cases of H. influenzae, with 316 reported cases impacting children under the age of five. Of the infections reported in children under five years of age, only 15 cases were confirmed as H. influenzae type b. The number of H. influenzae type b infections in persons five years of age and older is not known.
Currently, among all age groups, nontypeable H. influenzae is responsible for the majority of invasive disease and non-b type H. influenzae infections have become more prevalent than type b. Hib vaccine does not prevent invasive disease cause by nontypeable and non-b types of H. influenzae.
Globally, in 2015, there were an estimated 340,000 cases of severe H. influenzae type b infection, and 30,000 Hib related deaths. Countries noted to have the highest rate of Hib infections included China, India, South Sudan, and Nigeria. Between 2000 and 2015, deaths from Hib were reported to have dropped by 90 percent globally.
IMPORTANT NOTE: NVIC encourages you to become fully informed about Haemophilus Influenzae Type B (Hib) and the Hib vaccine by reading all sections in the Table of Contents, which contain many links and resources such as the manufacturer product information inserts, and to speak with one or more trusted health care professionals before making a vaccination decision for yourself or your child. This information is for educational purposes only and is not intended as medical advice.



